Contributed by Bob Rawlins, consultant to CAIRE Inc. ~
How many are with me? 2021 has been a tough year for many. COVID finding new strain variances has not helped either.
I’ve always been the type of person that doesn’t want to wish the time away. Time is so precious. How many times can you remember saying things like, this is the longest day. I wish this week would end already. Or, 2021 can’t get over fast enough.
I really don’t like wishing the time away. But this year offered difficulties for all of us.
My journey started six years ago when an infectious virus got into my body and decided to attack the lungs. From that first day I went into the ER I was on 3-4 Liters of oxygen therapy 24/7.
It was an idiopathic virus that the best of infectious diseases doctors could not label. After 42 infectious disease tests, still unknown. However, the scarring was real.
Unfortunately, the scarring was mostly in the lower part of the lungs, and it really caused havoc with breathing and oxygen transferring properly throughout my body. Hence, 24/7 oxygen and adjustments up depending on the activity I was performing.
Fortunately, for about four years I remained stable. I was able to do many things and managed my oxygen needs. Once I got my CAIRE portable oxygen concentrators (POCs), I became even more mobile and more flexible with activities. I was still able to coach soccer, went snow skiing, walked a 5K, and traveled to get as much normalcy in my life as possible. So, if you are on oxygen, find a way to become more mobile to help you mentally and give you the confidence to live your life as best you can.
Over the last two years, my symptoms became more of a concern to my team of doctors and caregivers. My doctor referred me to the lung transplant team, which was preceded by two years of testing and evaluation meetings with some top doctors in their field.
If your pulmonologist has suggested lung transplant evaluation, I would encourage you to do so. You can always say no. But with chronic lung disease you must make sure you are going after all the ways to help you improve your quality of life. It’s a big decision.
Remember however, fibrosis, scarring, won’t get better — it will continue to progress. That to me was my biggest fear. All the tests you do can’t accurately predict how fast it will progress. I didn’t want to get too sick that lung transplant was off the table.
Cleveland Clinic monitored me very closely during this period of time. I was going for all my lung tests and blood work every two months. Then, the day of decision came.
I remember the day my lung transplant doctor told me it was time to get on the waiting list for a double lung transplant.
My wife and I started to cry. We were anxious, nervous, and in shock, I think. I am an optimistic person. From day one I was determined to do whatever I could to get back to normal and off oxygen. That wasn’t going to happen. ☹
So, after much reservation and lots of questions, we decided to get listed. Our family had some reservations, but that’s normal. In the end, I decided to listen to those much smarter than me to try and give me my best quality of life.
So, I was listed in July of 2021. And the waiting began. I got on several support groups like, Right 2 Breath, Lung Transplant Recipients, Transplant Talk, and Second Wind Lung Transplant Association, Inc.
In just three months I got a call that they have found some potential lungs for me. Talk about all the feelings that go through your head in that moment is indescribable.
As we approached the hospital emotions of being scared, excited, uncertain, and anticipation were present. Then when this first call ended up being a “Dry Run,” we felt disappointment. When you have a dry run, they prepare you right up until they are ready to take you into the operating room. Unfortunately, this wasn’t the time for me. So after almost 12 hours of waiting we went home to wait for the next call.
About a month later it came. Here we go again, off to the hospital. This felt different. This was going to be my turn. At 10 AM they took me into the operating room, and I came out about 6 PM.
I would be in the ICU on a ventilator for just 12 hours. That was a great sign that things went well, they explained. (I was on one of those strong hospital cocktails that leave you sleeping for a while. 😊)
This is where things really begin on this new journey. At first, I felt like I couldn’t breathe properly, couldn’t get that deep breath in. My oxygen levels were great but that anxiety of feeling like I couldn’t breathe was there. The team said it will take some time and you’ll have to learn to breathe again with the new lungs. The brain must recognize that you are no longer breathing on bad lungs. This was just bizarre — the body is so complex.
Pain is real, but they provide you all the comforts for that. Having seven tubes in your body for draining the fluids after surgery is surreal. I was the new 6 million dollar man. My doctor said I am now “healthy, complicated.”
You must keep your strength up before transplant and I learned quickly why. You will lose some muscle weight. Being in the best shape is key.
I kept pushing physical therapy, walking and any exercise I could do before surgery, and I am really glad that I did.
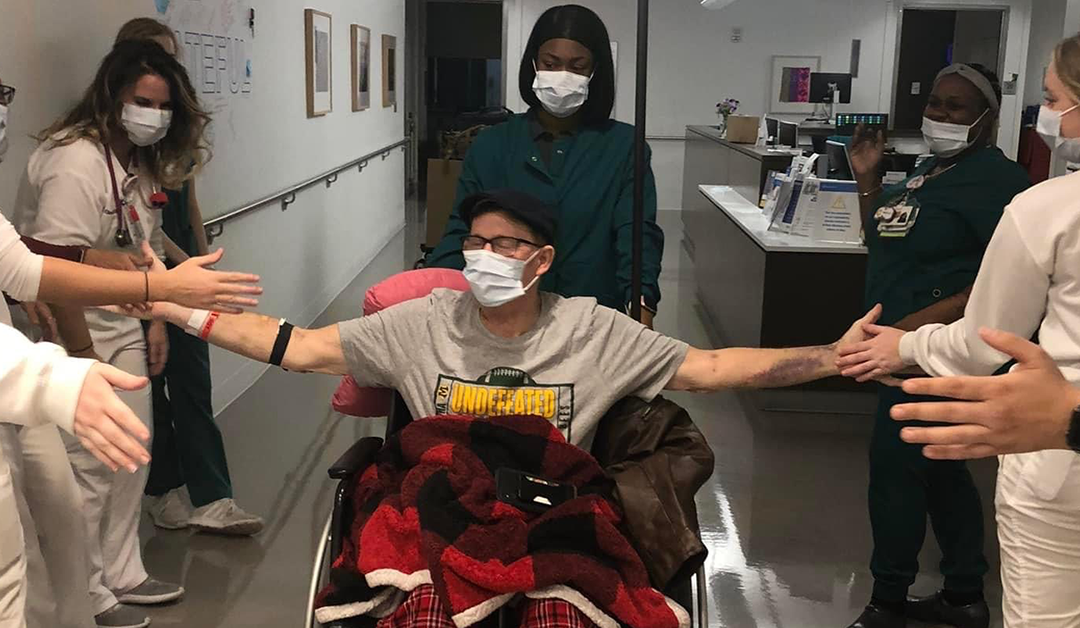
In 11 days, the lung transplant team released me from the hospital after the most difficult and complicated surgery to date. The best part, I am off supplemental oxygen and working on the healing process. It is a long recovery but it’s so worth it.
So, there are parts of 2021 that I am happy are over with, and I want to move on. 
I’m looking to do some catch-up of many things I couldn’t do in 2021 and before. 2022 is going to be good to all of us my friends. Our nation and nations around the world have suffered and it’s time to turn the corner to recovery.
Do your part, stay healthy and safe so you can help keep others the same way.
Happy New Year!!!!
Love you all and praying for all of you to have a safe and healthy new year and beyond!
God Bless
Till next time,
Coach Bob, (without supplemental oxygen)
#doyourpart
#breathe-easy
#smileeveryday
#touchaheart
Bob Rawlins, 64, of Medina, Ohio, is a double lung transplant recipient and a patient advocate for those who suffer from respiratory diseases and have been prescribed supplemental oxygen therapy. He is husband to Terese and father to their 17-year-old triplets. He also has two grown twin sons and four grandchildren. He serves as a hospital volunteer, band dad and chaperone, and marketing guru.
If you have been prescribed oxygen therapy, learn more about CAIRE by visiting www.caireinc.com/patients or by calling 1-800-482-2473 to talk to an oxygen advisor.
The contents of this blog post are not intended to substitute for professional medical advice. Please consult your physician for personalized medical advice. When using any oxygen therapy device please consult the applicable product instructions for use for product indications, contraindications, warnings, precautions, and detailed safety information.